{Page 3}
Switching on color Doppler in the apical 4-chamber view (Figure 6) we can see mitral regurgitation with central origin and a small flow velocity convergence area. In the parasternal long-axis vew (Figure 7) the regurgitant jet appears smaller, because the jet area is displaced medially, towards the interatrial septum (Figure 6).
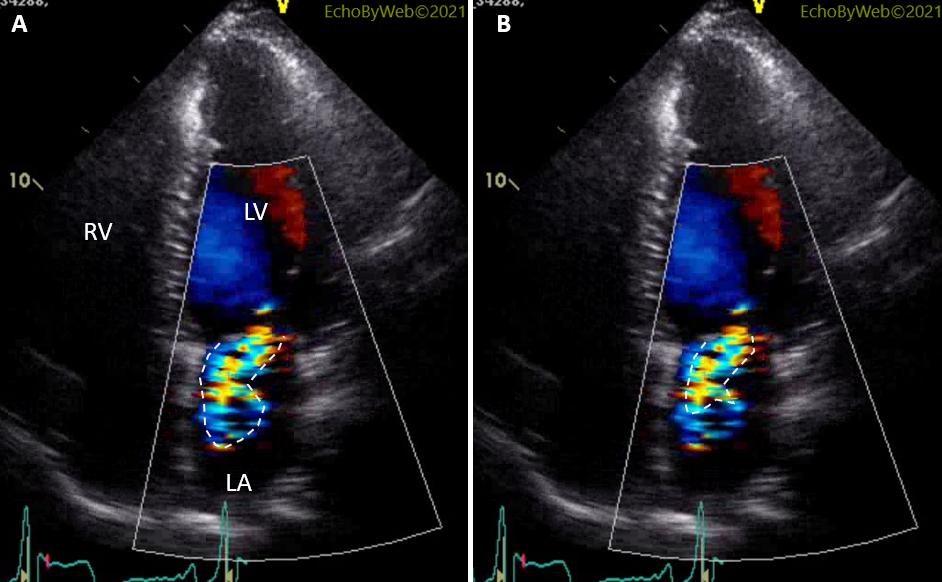
A simple way to grade mitral regurgitation is to consider the area occupied by the jet in the atrial cavity, especially if related to the area of the atrial cavity. A semi-quantitative measure can be obtained by planimetry of the jet. In Figure 8, 2 very different jet areas are obtained by planimetry: in A, planimetry is performed encircling all the color Doppler area, and this results in estimating a moderate regurgitation; in B, planimetry considers only the aliasing velocity (red blood cells with velocity > 70 cm/s), and this results in estimating a mild regurgitation. In this latter case, we are looking only at accelerated blood cells coming from the LV cavity (= regurgitant volume); in the former case, we are including also low-velocity blood cells which were in the left atrial cavity, and are displaced by the blood cells coming from the left ventricle. In other words, in A we are over-estimating mitral regurgitation.
Although this method is widely used to “eyeball” mitral regurgitation, it is discouraged by the Guidelines because it is dependent on too many factors which are not related to the grade of regurgitation (ultrasound penetration, color gain setting, the direction of the jet relative to the direction of the ultrasound beam – just to mention a few). Most importantly, color Doppler is related to the velocity of the jet and its penetration in the atrial cavity (which is related to the left ventricular – left atrial pressure difference) and not to the number of blood cells entering the left atrium (= regurgitant volume).